Cirrhosis Of The Liver
Cirrhosis of the liver is the term used to describe liver disease where chronic inflammation of liver cells has caused an extensive and widespread build up of scar tissue in the liver. Scar tissue is similar to collagen, as it is tough fibrous tissue, which replaces damaged liver cells. This scar tissue is not functional and cannot do the work of liver cells.
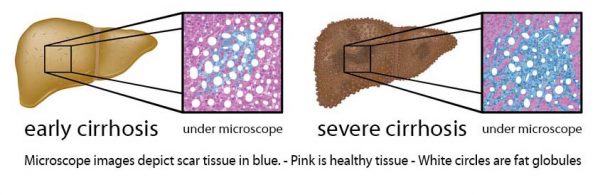
What causes cirrhosis of the liver?
Liver cells known as stellate cells produce the scar tissue to protect themselves from the inflammation that is occurring in the liver. This inflammation is produced by free radicals generated by various liver toxic factors operating over many years.
A healthy liver does not have many stellate cells and they do not produce excessive amounts of scar tissue. In contrast, in a liver that is chronically inflamed, the stellate cells become activated and they multiply and produce excessive collagen.
A cirrhotic liver is hardened with scar tissue, which reduces its blood supply. There is not enough healthy liver tissue remaining to perform the metabolic and detoxification processes that the liver must perform to keep the body healthy.
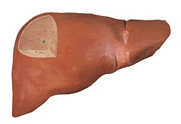 |
 |
| A normal healthy Liver | Liver affected by Cirrhosis |
Cirrhosis of the liver is the fourth most common cause of death among people aged between 30 and 50. Chronic hepatitis (caused by the hepatitis B and C viruses) is gaining on alcohol as the leading cause of cirrhosis.
The most common causes of cirrhosis are –
- Excessive alcohol
- Chronic hepatitis B and C infection
- Autoimmune liver diseases such as autoimmune hepatitis and primary biliary cirrhosis (PBC)
- Genetic disorders of metabolism such as hemochromatosis (iron overload) and Wilson’s disease (copper overload)
- Adverse reactions to some drugs such as methotrexate, analgesics and statin drugs etc.
- Fatty liver of moderate to severe degree
- Vascular disorders of the liver
Signs of advanced cirrhosis of the liver may include
- Spider nevi – spider shaped tiny blood vessels (capillaries) on the skin
- Excessive bruising
- Jaundice (yellow discoloration of skin and eyes)
- Altered liver size
- Enlarged spleen
- Clubbing of the ends of the fingers
- Ascites (extreme build up of fluid in the abdominal cavity)
- Swelling of the legs with fluid (edema)
- A flapping tremor of the hands
- Mental confusion and disorientation
- Vomiting of blood from varicose veins in the esophagus (esophageal varices)
Nutritional medicine for cirrhosis
Increase antioxidant intake, to reduce damage to liver cells from free radicals.
The most important antioxidants include –
- Vitamin E 1000 IU daily (some people may need 2000 IU)
- Vitamin C 1000 mg twice daily
- Selenomune 200 – 300 mcg daily
Vitamin E is able to reduce the ability of the stellate cells to manufacture collagen and so reduces scar tissue production. Vitamin E can also soften existing scar tissue and therefore improve blood flow to the liver, which is essential for regeneration of the liver cells. Vitamin E assists in the maintenance of high levels of glutathione, which is the most powerful liver antioxidant to prevent cirrhosis. A clinical study of hepatitis C sufferers not responding to interferon therapy, showed that nearly 50% improved dramatically with 800 IU daily of vitamin E. These are the reasons why a high dose of vitamin E is required. Use only natural vitamin E which is known as d-alpha tocopherol.
It is vital to obtain plenty of beta-carotene and its related carotenoids from eating a wide variety of raw brightly colored fruits and vegetables. Beta-carotene is converted in the body to vitamin A. Beta-carotene, other carotenoids and vitamin A, have a powerful anti-cancer effect in those with cirrhosis. This will reduce the risk of cirrhotic livers developing cancer. Those with liver disease need to be careful not to take excessive amounts of vitamin A and should not take more than 10,000 IU daily.
Selenium has been shown in clinical studies to reduce the incidence of liver cancer and should be taken daily by those with cirrhosis and/or other risk factors for liver cancer. For more information see the website www.seleniumresearch.com
Take a liver tonic that contains the essential nutrients to support the liver’s ability to break down and excrete toxins. This will reduce the damage that toxins can inflict upon liver cells and support the repair of damaged liver cells. For cirrhosis, I would recommend a daily liver tonic that contains Milk Thistle, B vitamins, sulfur containing amino acids and selenium.
N Acetyl Cysteine (NAC) should be taken in a dose of 600 mg three times daily to help the damaged liver to make more glutathione.
Vitamin K – many people with cirrhosis have a problem with bruising or bleeding from enlarged veins in the esophagus. This is because the damaged liver cells are unable to manufacture sufficient amounts of clotting factors. This can be helped by the daily consumption of a fresh juice made with a mixture of raw dark green leafy vegetables. Good vegetables to use for this purpose are spinach, kale, beetroot tops, parsley, mint, watercress, wheatgrass and alfalfa sprouts which are high in vitamin K. Vitamin K will help to reduce this deficiency of clotting factors and will reduce bruising and bleeding.
General measures for cirrhosis of the liver
- Minimize the use of all medications, especially liver toxins such as alcohol, analgesic drugs (especially acetaminophen, paracetamol and narcotics) and anti-inflammatory drugs. Avoid using household and workplace chemicals such as insecticides, pesticides, chlorine, bleach, paints, glues and solvents.
- Protein intake – the cirrhotic liver cannot handle large amounts of concentrated protein at one time and for this reason minimize the consumption of red meat and poultry. If you eat too much animal protein, ammonia levels will build up in the bloodstream causing fatigue and mental confusion. Selenomune and N Acetyl Cysteine (NAC) supplements help to reduce ammonia levels in the body. Suitable protein sources are legumes (beans, peas and lentils), grains, cereals, seeds, sprouts and nuts.
- Avoid constipation by consuming plenty of raw fruits and vegetables, and grind fresh seeds (flax seeds, pumpkin seeds, sunflower seeds etc) and almonds to increase intestinal fiber. Fibertone powder is excellent to increase necessary fiber bulk in the bowel. This increased fiber will speed the passage of toxins out of the bowels and reduce the ability of these toxins to re-circulate back to the liver. The laxatives Osmolax and Lactulose are also good products to draw fluid into the bowel to ease constipation.
- If bowel function is poor because of constipation with high amounts of bacteria in the bowel, this can lead to excessive fermentation of the bowel contents, which will increase absorption of toxic ammonia from the bowel. A healthy liver can convert nitrogen into urea, which is excreted in the urine. In patients with end stage cirrhosis and very poor liver function, the liver is not able to handle these high levels of ammonia and toxic brain symptoms may occur. In this situation, bowel function should be improved by increasing raw food fiber and taking supplements of the healthy lactobacillus bacteria. Enemas and colonic irrigations can also help if there is severe constipation and auto-intoxication from the bowel.
- Fifty percent of your diet should consist of raw and cooked vegetables and fruits. Dressings can be made with organic apple cider vinegar and cold pressed olive oil. Drink one or two glasses of raw vegetable juices daily.
- Eat cruciferous vegetables including broccoli, cauliflower, Brussels sprouts, kale, cabbage, Bok choy and watercress, as well as garlic and onions to help the detoxification ability of the liver.
- Ask your doctor to check that your body’s total iron content is within normal limits. This can be confirmed with a simple blood test known as serum iron studies. Excess iron can increase liver damage and cause cirrhosis. If your iron levels are excessively high, avoid iron-enriched cereals and vitamin pills containing iron and liver.
Conclusion
Liver disease is serious and requires treatment and regular monitoring by a liver specialist.
A liver specialist is known as a hepatologist and you need to be referred by your family doctor or general practitioner. Over nearly 40 years of practicing medicine I have seen many patients develop severe liver disease, which sadly could have been prevented by early detection and early referral to a hepatologist. There needs to be more awareness of liver disease so that patients can be treated early so that we can prevent cirrhosis, liver failure and liver cancer. Make sure you have your liver function checked annually with a blood test.
I have presented my ideas on how to help those with liver diseases using nutritional medicine, which I have been using for many years with good success rates. However, my recommendations do not replace the care of your own doctor and you should remain under the care of your own doctor whilst using nutritional therapies.
If you have any questions you may contact my naturopath, Christine, on 623 334 3232 or email us at support@liverdoctor.com
The above statements have not been evaluated by the FDA and are not intended to diagnose, treat or cure any disease.


Thank You so much for the Information Dr.Sandra Cabot. I am having Cirrhosis of the Liver as I have been taking Medication for Bypass Surgery. Appreciate very much if you could please recommend some Medicine to reduce the scarring.
My Email : lakmaaldezoysa14@gmail.com
Kind Regards
Lakmaal De Zoysa from Srilanka
Hi Lakmaal,
Thank you for reaching out.
Are you in Australia?
Kind regards,
Jessah Shaw
Nutritionist
Hi Jessah Shaw,
I live in Srilanka, and appreciate very much if you could please advise me as I have pain on and off on the upper right side of my stomach, and is it due to Liver Cirrhosis.
I started taking Cabot Health Liver Tone Shots Ultra Potent Tablets once a Day to Cleanse & Detox the Liver. What should I eat on a daily basis, and how do I cure my right side stomach pain.
Looking forward to hearing from you ASAP.
Kind Regards,
Lakmaal De Zoysa from Srilanka.
Email: lakmaaldezoysa14@gmail.com
Hi Lakmaal,
You may find this article on cirrhosis helpful: https://www.liverdoctor.com/cirrhosis-how-can-we-help-it/
To boost liver health and your vitality, Dr Cabot prescribes
Livatone Plus – 1 cap twice daily for 2 weeks and then increase to 2 capsules twice daily, to improve liver function. Livatone contains milk thistle and selenium (Commence this after finishing the Livatone Shots).
N-Acetyl-Cysteine (NAC 600mg) – 1 cap twice daily for 2 weeks and then increase to 2 capsules twice daily well away from food, if any upset occurs take at the beginning of your meals. NAC should be taken with a whole glass of water away from food. Do not take just before retiring to bed. NAC can be strong on the stomach, and this is why you need to take it with a whole glass of water. This supplement works well with Livatone Plus to get your liver better faster. This supplement is the precursor nutrient of glutathione; the body’s strongest anti-oxidant.
You may purchase these supplements and Dr Cabot’s books at https://shop.liverdoctor.com/
To soften the liver scarring and resolve cirrhosis as much as possible, Dr Cabot prescribes
Serrapeptase – begin with 1 capsule daily for 3 days, increase to 1 capsule twice daily for 4 days and if it well tolerated you may increase the dose to 2 capsules twice daily and always to be taken on an empty stomach. Care to be taken with this supplement if you have liver related bleeding problems or if you are taking blood thinners.
Vitamin E – 1 capsule twice daily, to soften scar tissue. Care to be taken if you have bleeding concerns or if you are taking blood thinning medication.
You may purchase these supplements and Dr Cabot’s books at https://shop.liverdoctor.com/
We recommend our free liver diet guide here: https://www.liverdoctor.com/liver-diet-guide-free-download/
Kind regards,
Jessah Shaw
Nutritionist
Hi, I have compensated cirrhosis caused by Alcohol, I have given up Alcohol and am currently being treated at the RPA Liver Clinic Sydney.What more can I do for my health. Thanks
Hi Alex,
Thank you for your email.
You may find these articles helpful:
https://www.liverdoctor.com/cirrhosis-how-can-we-help-it/
https://www.liverdoctor.com/natural-ways-to-fight-addiction/
We recommend checking out Dr Cabot’s liver videos here: https://www.youtube.com/@drsandracabot/search?query=cirrhosis
In addition to the Livatone Plus to boost liver health and your vitality, Dr Cabot prescribes
N-Acetyl-Cysteine (NAC 600mg) – 1 cap twice daily for 2 weeks and then increase to 2 capsules twice daily well away from food, if any upset occurs take at the beginning of your meals. NAC should be taken with a whole glass of water away from food. Do not take just before retiring to bed. NAC can be strong on the stomach, and this is why you need to take it with a whole glass of water. This supplement works well with Livatone Plus to get your liver better faster. This supplement is the precursor nutrient of glutathione; the body’s strongest anti-oxidant (You will need to call us on 02 4655 4666 to order this as it is practitioner-only).
Glutamine – a heaped teaspoon of glutamine throughout the day, any time you get a craving. Glutamine is an amino acid best known for healing a leaky gut and increasing muscle mass in athletes. Glutamine also helps reduce cravings for sugar and alcohol.
Tyrosine – 1 tsp when you experience cravings for sugar and alcohol. Effects last about 4 hours. Tyrosine is required for the manufacture of dopamine and noradrenaline, which are required for concentration, alertness, memory and a happy, stable mood. This will assist in balancing your brain chemistry.
Kind regards,
Jessah Shaw
Nutritionist
Hello,
My name is Michelle I have cirrosis of the Liver due to excessive alcohol intake. The scarring is accute and my spleen is enlarged. I am being monitored by a gastroenterologist and a blood specialist every 6 months. What do you recommend by way of suppliments?
Hi Michelle,
You may find this article on cirrhosis helpful: https://www.liverdoctor.com/cirrhosis-how-can-we-help-it/
Plus this article on addiction: https://www.liverdoctor.com/natural-ways-to-fight-addiction/
We recommend checking out Dr Cabot’s liver videos here: https://www.youtube.com/@drsandracabot/search?query=cirrhosis
Where are you located?
Kind regards,
Jessah Shaw
Nutritionist